
EDUCATION

Understanding EGFR-Positive Lung Cancer
WHAT IS EGFR-POSITIVE LUNG CANCER?
HOW LUNG CANCER BEGINS
WHO’S AT GREATEST RISK FOR EGFR+ LUNG CANCER?
EGFR+ SYMPTOMS, DIAGNOSIS AND TESTING
REFERENCES
HOW DO CANCER CELLS DIFFER FROM NORMAL, HEALTHY CELLS?
HOW LUNG CANCER GROWS AND SPREADS
WHAT CAUSES EGFR+ LUNG CANCER?
EGFR+ LUNG CANCER TREATMENT OPTIONS
WHAT IS EGFR-POSITIVE LUNG CANCER?

Around 15% of all lung cancer patients in the United States are diagnosed with EGFR-positive (EGFR+) lung cancer, with prevalence among people of Eastern Asian descent falling between 35 – 50%.
EGFR-positive lung cancers are a family of lung cancers that test positive for an EGFR gene mutation. EGFR is an acronym for epithelial growth factor receptor, a protein present on the surface of all cells — both normal, healthy cells and cancer cells.
An EGFR mutation is a damaging change to the part of a cell’s DNA that carries the recipe for making these EGFR proteins.
Recent advances in our understanding of how cell signaling, or communication, pathways regulate cell behaviors have identified genetic aberrations that can suppress cell death, promote cell division, and ultimately, produce tumors. EGFR is one of those discoveries.
HOW DO CANCER CELLS DIFFER FROM NORMAL, HEALTHY CELLS?
First, it helps to understand how proteins in our bodies regulate cell growth…
The nucleus (center) of each of our cells contains our genetic material, or DNA. These genes act as the blueprint — a sort of genetic instruction manual — for all of the proteins produced in our bodies should behave. Some of these proteins are growth factors (e.g., EGFR), chemicals that tell cells to divide and grow. Others suppress or inhibit growth.

Mutations in certain genes — for example, mutations caused by tobacco smoke, radiation or other carcinogens — can trigger abnormal protein production… too many or not enough proteins, or abnormal, malfunctioning proteins.
If a gene carrying the instructions for creating EGFR proteins is damaged or mutated, abnormal proteins are produced. These abnormal proteins, in turn, function abnormally when performing their job of regulating cellular growth.
You can think of the EGFR protein as an ON-OFF switch. When growth factors (tyrosine kinases, in the case of EGFR+ lung cancer) attach to the EGFR protein on the surface of a cell, a signal is sent to the cell’s nucleus telling it to grow and divide. But in some cancer cells, this protein is overexpressed and the switch remains stuck in the ON position, telling these cells to keep growing and dividing, even when they should otherwise stop because enough cells are present. Sustained activation yields more aggressive tumor phenotypes.1
This EGFR mutation has now become what’s known as an “activating mutation.” It can activate cell-survival signals, leading to increased cancer cell proliferation. Identifying activating mutations is thought to be the most important predictor of how well a patient will respond to TKIs, or tyrosine kinase inhibitor medications.18
HOW LUNG CANCER BEGINS
Lung cancer usually begins several years before it’s diagnosed, before it even causes symptoms. Cells in the lungs become cancer cells after undergoing a series of mutations that transform them into cancer cells. Lung cancer begins — that is, a tumor originates — when a mass of cancer cells effectively becomes “immortal.” The math — the division and multiplication of these cells — is out of control.

HOW LUNG CANCER GROWS AND SPREADS
In the normal, healthy body, roughly three billion cells divide every single day. “Accidents” in cell reproduction triggered by genetic abnormalities or environmental carcinogens during any of those cell divisions can result in a cell that, after further mutations, can develop into a cancer cell.
One of the differences between benign lung tumors and malignant lung cancer is that lung cancer cells have the ability to break off and spread to other regions of the body. This ability to spread is actually the cause of most cancer deaths.
One difference between cancer cells and normal cells is that cancer cells lack “stickiness.” Normal cells produce substances (adhesion molecules) that cause them to stay together. Without this stickiness, lung cancer cells can break away to travel and grow in other regions, as well as invade nearby structures.
Lung cancers spread in the following ways:
- Invading tissues locally or regionally. Unlike benign tumors which may push up against nearby tissues, cancers actually penetrate nearby tissues. The name cancer is actually derived from the Greek word for “crab.” Cancerous masses can penetrate nearby tissues with crablike extensions.
- Lung cancer cells can break away and travel around the body through the bloodstream.
- Lymphatic system. After expanding locally, cancers tend to spread to nearby lymph nodes, first through the lymph channels.
- Pulmonary airways. Lung cancer may travel and spread through airways in the lungs.
Where does lung cancer spread or metastasize? The most common sites of metastasis (development of secondary malignant growths distant from the primary site of cancer) include the brain, bones, liver, and adrenal glands. Lung cancer is somewhat unique in that it can also spread to the bones of the hand and feet.
Now, considering that we experience three billion cellular divisions on a daily basis, you may be wondering why there aren’t more “accidents”… why doesn’t everyone develop cancer? The answer is that our normal cells are regulated by a series of checks and balances. It’s actually very difficult for a normal cell to become cancerous. It must first evade multiple checkpoints.
For example, it must:
- carry growth factors that prompt it to grow even when growth is unnecessary
- evade proteins that direct it to stop growing, and die when it becomes abnormal
- ignore signals from neighboring cells that are telling it: “Hey, you’ve reached your boundary!”
- lose the “stickiness” (adhesion molecules) that normal cells produce, allowing it to float away to nearby locations, or through the bloodstream or lymphatic system to distant areas in the body. (For example, heart cells stick to other heart cells and don’t travel to the foot. Normal lung cells remain in the lungs unless they lose their adhesion molecules.)
In reality, however, lung cancer is a complex disease, and it’s usually a combination of abnormalities that produces a cancerous cell, rather than a single mutation or protein abnormality.


WHO’S AT GREATEST RISK FOR EGFR+ LUNG CANCER?
EGFR mutations are most common in people with lung adenocarcinoma, a type of non-small cell lung cancer (NSCLC) involving a malignant tumor formed from glandular structures in epithelial tissue. (Adenocarcinomas are also referred to as non-squamous non-small cell lung cancer.)
Around 85% of all lung cancers are non-small cell lung cancers, and over half of these are adenocarcinomas.
While it may be possible for anyone to develop the EGFR driver mutation for lung cancer, certain populations may be at greatest risk…
Never-smokers. It’s important to be aware that EGFR mutations are more common in never-smokers (people who have smoked 100 or fewer cigarettes over their lifetimes2), non-smokers and light smokers. In fact, while around 15% of overall lung cancer patients express the EGFR mutation, lung cancers in non-smokers and never-smokers are far more likely to have this mutation.
This never-smoker trend is echoed in the overall population of lung cancer patients. Around 70% of those who develop lung cancer are never-smokers, and around two thirds of those never-smokers are women.
EGFR-positive lung cancer is also more common among:
- young adults with lung cancer. EGFR mutations are present in roughly 50% of lung cancers in young adults.
- people of East Asian ancestry
- Caucasians than African Americans
- women than men. While once considered a “man’s disease,” lung cancer, overall, is the leading cause of cancer deaths in women, killing more women each year than breast cancer, uterine cancer, and ovarian cancer combined. Lung cancer occurs at a slightly younger age in women than in men, and almost half of lung cancers in young adults occur in women.
WHAT CAUSES EGFR+ LUNG CANCER?
The etiology, or causes, of EGFR-positive lung cancer still remain largely shrouded in mystery. It’s important to remember that lung cancer is a multifactorial disease, which means that often, several risk factors combine to cause cancer.
Research, so far, has implicated several possible culprits…
Gene Mutations
Gene mutations (changes in the DNA of cells) can be a hereditary predisposition. A genetic predisposition is a genetic variation that increases the likelihood of a disease and is passed on from parents to children, although not all children will necessarily receive the gene types that will predispose them to a particular disease. Usually, a genetic predisposition is due to one or more gene mutations that have been passed on through generations.
Gene mutations can also be acquired; that is, genes can be damaged as a result of exposure to environmental carcinogens (cancer-causing substances).
This accumulation of mutations is one explanation for why many people develop lung cancer though they’ve never smoked, and some people smoke throughout their entire lives and never develop lung cancer.
(For an in-depth look at EGFR genetic mutations, see the Diagnosis and Testing sections.)
Environmental
There are many possible environmental carcinogens that can cause or contribute to lung cancer. Following are some of the key culprits…
Radon. According to the National Cancer Institute (National Institutes of Health), exposure to radon in the home is the second-leading cause of lung cancer, and the leading cause in non-smokers. It’s estimated that around 21,000 people develop lung cancer from radon exposure each year. Radon, a radioactive gas produced by the natural decay of uranium in the soil, can seep into homes through cracks in the foundation, around sump pumps, drains and through gaps around pipes and wires.

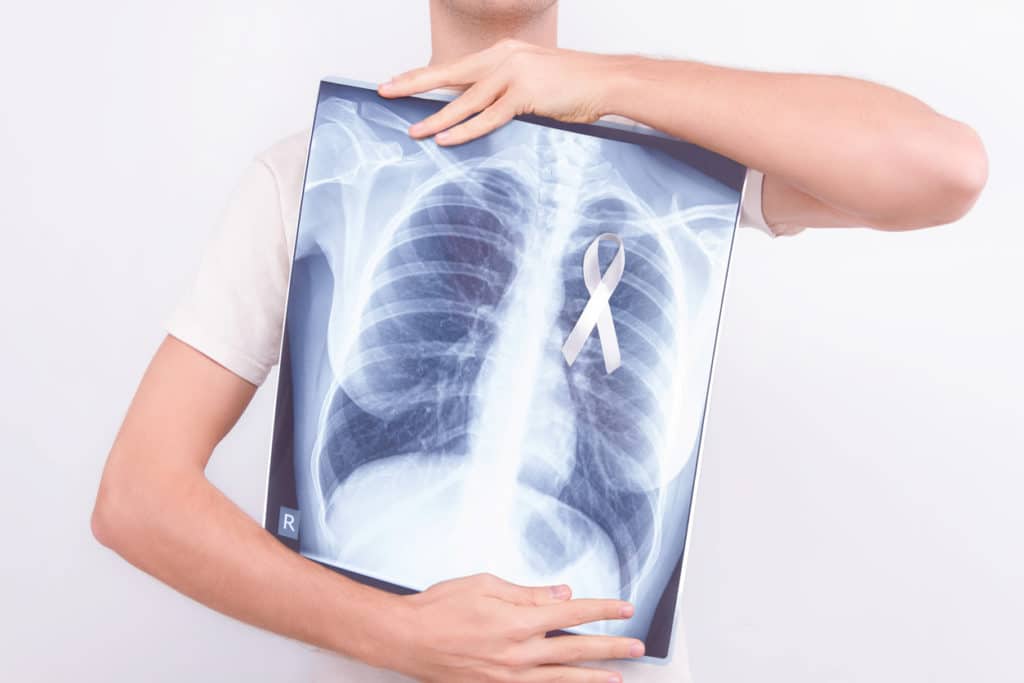
In the U.S., a radon level over 4pCi/L (pico curies per liter) is considered abnormal and should be repaired immediately. According to the Environmental Protection Agency, a radon level of 4pCi/L is considered five times more likely to result in death than the risk of dying in a car crash. About 1 in 15 U.S. homes is estimated to have radon levels at or above this EPA action level.
For more, see the EPA Consumer’s Guide to Radon Reduction. Or contact: National Radon Hotline, 1-800-767-7236; National Radon Helpline, 1-800-557-2366; National Radon Fix-It Line, 1-800-644-6999.
Asbestos. Exposure to asbestos is often considered to be an occupational exposure, but working with asbestos insulation in older homes (built prior to 1970) can result in exposure, too. Asbestos is responsible for roughly 84% of cases of mesothelioma, a cancer that affects the lining of the lungs, and is responsible for other forms of lung cancer, as well. Left alone, asbestos poses little danger, but when disturbed, it becomes dangerous.
Air Pollution. Because lung cancer is more prevalent in urban areas than rural areas, air pollution is often investigated as a possible risk factor for lung cancer. At the least, air pollution is believed to contribute to oxidative stress — damage to the cells caused by oxidation — which is known to play a role in the cancer disease process. While there doesn’t seem to be a consensus on the degree to which air pollution contributes to lung cancer in the U.S., large studies of lung cancers in Europe suggest that up to 10.7% of lung cancers in never-smokers may be caused by air pollution, according to Cancer Research UK.
Industrial Chemicals. Certain products used in the home (e.g., wood strippers) contain chemicals associated with an increased risk of lung cancer.
Radiation Exposure. Exposure to medical radiation to the chest for other cancers (e.g., Hodgkin’s lymphoma, breast cancer) can increase the risk of seoncary lung cancer, although the benefits of treatment may outweigh this risk.17
Wood Smoke. Exposure to wood smoke may increase the risk of lung cancer. Converting from wood-burning stoves and fireplaces to other options (e.g., gas fireplaces) can help reduce this risk.
Secondhand Cigarette/Cigar Smoke — According to the American Lung Association, smoke emitted from tobacco contains about 70 toxic chemicals that are known to be linked to cancer (carcinogenic). Poisonous chemicals such as benzene, formaldehyde, vinyl chloride, arsenic ammonia, hydrogen cyanide, and carbon monoxide are released into the air by smokers.


Occupational Exposure
The following lists of substances and occupations provide an overview of some of the most common occupational exposures that have been linked to lung cancer.
Lung Cancer-Linked Substances
- Arsenic (involved in textiles, ceramics, glassware production, fireworks, semiconductors)
- Radon
- Solvents (e.g., benzene, toluene)
- Reactive chemicals — bis(chloromethyl) ether, mustard gas, vinyl chloride
- Diesel fumes
- Natural fibers — asbestos, silica, wood dust (hardwoods more damaging than softwoods)
- Metals — aluminum, arsenic, beryllium, cadmium
Lung Cancer-Linked Occupations
- Aluminum production
- Asbestos workers
- Bartenders
- Ceramics
- Coal gasification
- Chemists
- Glass manufacturing
- Painters
- Printers
- Masonry workers
- Metalworkers (iron and steel foundry work)
- Sandblasters
- Rubber production
- Truck drivers
- Uranium miners
HPV (Human Papillomavirus) and EGFR Mutations
One 2018 meta-review of four studies investigating lung cancer in Asian countries found that the HPV infection was strongly associated with EGFR mutations in EGFR-positive lung cancer, especially in the Asian population.3 Overall, the EGFR mutation rate in this group was 38%, with an HPV infection rate of 35%.
EGFR+ SYMPTOMS, DIAGNOSIS AND TESTING
SYMPTOMS
Lung adenocarcinomas usually originate in tissues near the outer areas of the lungs and can be present for a long time before symptoms actually emerge. When symptoms do finally appear, they’re often less obvious than in other forms of lung cancer, manifesting with a chronic cough (e.g., lasting longer than eight weeks) and bloody sputum only later, in more advanced stages.
This is one of the reasons that lung cancer is often not diagnosed until the disease has, unfortunately, progressed to an advanced stage. This is especially true of young people and non-smokers or never-smokers who never imagined that they might have lung cancer.
In fact, studies have shown that 41% of patients diagnosed with NSCLC are not diagnosed until Stage IV.4
Early, more generalized symptoms such as fatigue, subtle shortness of breath, upper back and chest pain and unexplained weight loss may be easy to miss or attribute to other causes, such as asthma, bronchitis or acid reflux (gastroesophageal reflux disease, or GERD).


Diagnosis and Testing
It’s important for everyone with NSCLC — especially lung adenocarcinoma — to undergo genetic testing (also known as molecular profiling or biomarker testing) to detect genetic abnormalities in lung cancer cells. Molecular profiling is designed to reveal acquired gene mutations (somatic mutations), rather than hereditary gene mutations.
Gene testing requires obtaining a sample of the tumor; often, a sample of tissue is obtained during a lung biopsy. Samples can be obtained through a needle biopsy, during a bronchoscopy, through an open lung biopsy (during surgery), or through the more recently developed liquid biopsy — a promising new tool for detecting EGFR mutations.
Unlike the more invasive tissue biopsies, liquid biopsies only require a simple blood test. Liquid biopsies are still considered to be investigational, however, and are not used as the sole test to guide diagnosis and treatment of lung cancer. It’s hoped that, in the future, liquid biopsies will also provide an effective way to monitor EGFR-positive lung cancer patients in real time.
Currently, we only learn that a tumor has become resistant to EGFR treatments when it fails to respond, such as evidence of growing or spreading on lung scans. Liquid biopsies would enable us to learn that a tumor has become resistant sooner, which enables us to switch to a more effective therapy sooner.
Drivers and Passengers
Cancer cells can develop many mutations, but only a few are directly involved in the cancer process. These mutations lead to the production of abnormal proteins that guide the growth and development of a cancer cell. These abnormal proteins are known as driver mutations because they “drive” the growth and spread of cancer. Some, but not all, driver mutations are also “actionable mutations,” which means that they can be specifically targeted by a current medication.




Driver mutations are present in around 60% of people with lung adenocarcinoma.4 This percentage, as well as driver mutations in other forms of lung cancer, is likely to grow as our understanding of cancer pathology increases and we’re able to identify more mutations.
Driver mutations not only initiate the development of cancer, but work to maintain the growth of cancer as well.
Incidentally, in addition to EGFR driver mutations, which are the most common, the alphabet soup of other known genetic driver mutations associated with lung cancer include.4
- EML4 -ALK rearrangements
- KRAS mutations
- ROS1 rearrangements
- MET amplifications
- HER2 mutations
- RET rearrangements
- BRAF mutations
Types of Genetic Changes in Cancer Cells
There are many different types of EGFR mutations; that is, there are many ways in which EGFR can be changed genetically. These mutations vary both in terms of the type of mutation and the mutation’s location in a particular gene.
To understand molecular profiling and choosing targeted therapies for lung cancer, it helps to understand a few basic genetic principles. Genetic changes that may occur in cancer cells include:
- Mutations — a change in, or damage to, the DNA sequence of a particular gene
- Rearrangements — the sequence of DNA is rearranged
- Translocations — changes that occur when part of a gene on one chromosome is relocated to a different region of the DNA
- Gene fusion — A “fusion gene” occurs when a translocation brings together two genes that are ordinarily not together
- Amplification — the production of multiple copies of a gene; common in cancer cells
Different types of mutations include, for example:
- Point mutations — a mutation in which one base is substituted for another
- Deletions — a piece of genetic material is lost or deleted from the gene
- Insertions — a piece of genetic material is added to the gene
Passenger mutations, on the other hand, are like passengers in a car; they don’t drive cancer, but they’re along for the ride. Some tumors may have more than 1,000 of these mutations, although, in reality, we may not know exactly how many passenger mutations are present in a tumor, and the number varies from tumor to tumor.
Who Should Be Tested For EGFR Mutations?
The decision to test for EGFR mutations should be made by the treating physician as part of diagnosis. This decision may depend on the availability of sufficient tissue; therefore, it’s vital that biopsy methods are optimized and that tissue is conserved at initial diagnosis and whenever possible thereafter.
Although all patients with NSCLC may eventually be tested, the primary focus may need to be on patients with adenocarcinoma and/or patients with a non-smoking history since the frequencies of mutations are particularly high in these patients.
Both the identification of EGFR mutation and gene amplification status can be important in determining which tumors will respond to tyrosine kinase inhibitor medications.5
In EGFR testing, the available sample is usually paraffin embedded tissue. The use of primary tumor tissue is preferable, but when it’s not available, a sample from metastatic tissue may be obtained. Ideally, the tissue sample should contain at least 50% viable tumor cells.11
Mutation detection can be performed using a variety of mutation platforms. Direct sequencing is widely used (amplifying and sequencing EGFR exons 18-21). Other methods includes real-time-PCR (amplification refractory mutation system),11 high resolution melting analysis,11,12,13,14 and denaturing high performance liquid chromatography (DHPLS).11
Other tests, such as circulating tumor cell DNA tests, may provide a useful initial screening; however, circulating tumor cells are limited by numbers and difficult to extract.6
Immunohistochemistry (IHC) can be a useful prescreening test, in some cases, because it detects the most common and relevant mutations at the protein level (e.g., exon 19 deletions). But immunohistochemistry testing is limited in that it doesn’t detect all mutations.15,16
A cell’s surface may carry many antigens (toxins or other foreign substances) that trigger an immune response, such as the production of antibodies. Immunohistochemistry testing attempts to detect special antigens (e.g., proteins) in cells of a tissue section, following the rationale that antibodies specifically bind to proteins in biological tissues.
If you’ve been diagnosed with lung cancer, it’s important to talk to your oncologist about genetic testing. Although testing is now recommended for everyone with advanced NSCLC, a recent study reported that only 30- 60% of patients who meet testing criteria actually receive cancer susceptibility testing.7,8
Genetic testing is vital to obtaining the right diagnosis, thus ultimately, the right treatment. It’s a brave and promising new frontier that helps ensure precision medicine for every patient: the right patient receives the right medication at the right time.
Too complicated or not?




EGFR+ LUNG CANCER TREATMENT OPTIONS
Non-small cell lung cancer (NSCLC), which comprises about 75% of lung cancers, has historically proven difficult to treat because its pathological mechanisms were poorly understood.
Treatment options for EGFR-positive lung cancer generally include surgery, radiation, chemotherapy with a variety of medications, targeted therapies (as indicated by molecular profiling) and immunotherapy.
Alternative and complimentary treatments such as natural or herbal therapies, acupuncture and meditation may improve recovery, increase survivorship and quality of life, and help patients cope with cancer and cancer treatments. In fact, several studies have found that combination therapies targeting medication resistance are highly promising.5
There’s some good news for EGFR-positive lung cancer on the treatment front. Once upon a time, all lung cancer patients were offered the same blunt instrument of chemotherapy, which generally results in severe side effects and carries several risks in itself. Then doctors began genetically testing cancer patients to determine whether they had an EGFR (or other driver) mutation. And researchers began developing more precisely targeted therapies for these mutations.
The result has been a seismic shift in the way we manage lung cancer. Now, before starting treatment, lung cancer patients generally receive a complex and comprehensive genetic analysis to identify any driver mutations they may have.
There’s more good news. A mutation in a gene coding for EGFR is the most common “actionable” mutation among people with lung cancer. In other words, it’s the most common genetic change for which there are available treatments that directly target these lung cancer cells.
Tremendous advances have been made in the treatment of lung cancers with the EGFR molecular profile in recent years. Nearly half of CenterWatch’s 2018 FDA Approved Drugs for Oncology list target the EGFR molecular profile.9
Specifically, tyrosine kinase inhibitors (TKIs) directly target the EGFR protein in cancer cells, blocking the signals that travel to the cell nucleus and stopping growth of the cancer cell. These medications target cancer cells specifically and often have fewer side effects than traditional chemotherapy drugs, which target all rapidly growing cells. They directly target the activating somatic mutations of the tyrosine kinase domain of EGFR.11
In general, people usually don’t have more than one of these mutations. For example, it’s unlikely (though not impossible) for someone with an EGFR mutation to also have an ALK rearrangement or KRAS mutation in their lung cancer cells. And EGFR and KRAS mutations appear to be mutually exclusive.1
EGFR Inhibitors for Lung Adenocarcinoma
Currently, there are three FDA-approved TKIs for treating EGFR-positive lung adenocarcinoma:
- First-generation: Tarceva (erlotinib) and Iressa (gefitinib)
- Second-generation: Gilotrif (afatinib and dacomitinib)
- Third-generation: Tagrisso (osimertinib)
Third-generation TKIs, such as Tagrisso, also target EGFR-positive resistant lung cancer, inhibiting both EGFR-activating and resistance mutations.5
Treatment of Resistant EGFR-Positive Lung Cancer
Cancer cells are ever-evolving and, unfortunately, often develop mutations that make them resistant to drug treatments. There are several mechanisms by which patients can develop eventual drug resistance. But multiple mechanisms may be identifiable both upon repeat biopsy and in plasma circulating tumor DNA testing.
The EGFR T790M gatekeeper mutation — an exon 20 deletion — is responsible for 50-60% of these cases.5,11 This mutation affects the domain of EGFR that first- and second-generation tyrosine kinase inhibitors (such as Tarceva) bind to, making medications such as Tarceva, Gilotrif, and Iressa ineffective. Luckily, Tagrisso (osimertinib) is an option for those who develop a metastatic EGFR+ T790 mutation.
Yet, just as resistance develops with earlier-generation medications, acquired resistance to third-generation TKIs may develop, as well. Hopefully, drugs will continue to evolve to these treat resistant tumors so that more lung cancer survivors are living with lung cancer as a form of chronic disease, perhaps not cured, but controlled with these medications.
Which Treatment?
How do doctors determine which TKI will be the best first-line treatment for a specific patient’s EGFR-positive adenocarcinoma? Mutation testing can help determine the optimal treatment. But there may be many other factors that patients and their oncologists will want to consider.
Iressa has a reputation for having the fewest side effects and may be considered first choice for the elderly or someone with other major medical conditions requiring medication.
Gilotrif may be associated with greater side effects (especially mouth sores), but may also have a larger overall survival benefit. Gilotrif may also be a little more effective for people with an exon 19 gene deletion.
In the phase 3 FLAURA trial, Tagrisso (osimertinib), the newer, third-generation TKI, showed superior efficacy to that of Tarceva (erlotinib) and Iressa (gefitinib). Tagrisso almost doubled the median progression-free survival rate (duration of time in which the disease did not progress) — 18.9 months for patients taking Tagrisso compared to 10.2 months for patients taking Tarceva (erlotinib) and Iressa (gefitinib).
Tagrisso was shown to be able to affect only the target stated receptors and not the normal cells, which allowed it to actively and effectively treat the cancer with relatively minor side effects. The earlier generations of EGFR-positive drugs inhibit EGFR, but also inhibit some healthy cells, which leads to more side effects.19
Tagrisso is also currently considered to be the first-line treatment for EGFR-positive patients with brain metastases or leptomeningeal metastases, since it has a high rate of penetration into cerebrospinal fluid. (Many drugs are unable to reach the brain and spinal cord as they are unable to pass through the blood-brain barrier.)
The Bottom Line
Some of the most promising advances in lung cancer treatment have come from our enhanced understanding of genetic changes in lung cancer cells. In the past, we categorized lung cancers into a handful of types. But we’ve learned that no two lung cancers are exactly alike… if there were 20 people in a room with lung cancer, they would have 20 unique diseases, which may require 20 unique treatment plans.
The treatment landscape of EGFR-mutant lung cancer continues to evolve. Hopefully, that next breakthrough treatment that turns EGFR-positive lung cancer into a chronic, manageable disease is just one study away.
REFERENCES
- Bethune G, Bethune D, Ridgway N, Xu Z. Epidermal growth factor receptor (EGFR) in lung cancer: an overview and update. J Thorac Dis. 2010;2(1):48-51.
- Lovly, C., L. Horn, W. Pao. 2015. EGFR in Non-Small Cell Lung Cancer (NSCLC). My Cancer Genome https://www.mycancergenome.org/content/disease/lung-cancer/egfr/
- Hengrui Liang, Zhenkui Pan, Xiuyu Cai, Wei Wang, Chengye Guo, Jiaxi He, Yuehan Chen, Zhichao Liu, Bo Wang, Jianxing He, Wenhua Liang, on behalf of AME Lung Cancer Cooperative Group. The association between human papillomavirus presence and epidermal growth factor receptor mutations in Asian patients with non-small cell lung cancer. Transactional Lung Cancer Research. 2018:7(3).
- Zhu QG, Zhang SM, Ding XX, He B, Zhang HQ. Driver genes in non-small cell lung cancer: Characteristics, detection methods, and targeted therapies. Oncotarget. 2017;8(34):57680-57692.
- Barnes TA, O’Kane GM, Vincent MD, Leighl NB. Third-Generation Tyrosine Kinase Inhibitors Targeting Epidermal Growth Factor Receptor Mutations in Non-Small Cell Lung Cancer. Front Oncol. 2017;7:113. Published 2017 May 31. doi:10.3389/fonc.2017.00113
- Robert Pirker, MD,* Felix J. F. Herth, MD, PhD, FCCP,† Keith M. Kerr, MD, FRCPath,‡ Martin Filipits, PhD,* Miquel Taron, PhD, David Gandara, MD,¶ Fred R. Hirsch, MD,# Dominique Grunenwald, MD,** Helmut Popper, MD,†† Egbert Smit, MD, PhD,‡‡ Manfred Dietel, MD,§§ Antonio Marchetti, MD, PhD, Christian Manegold, MD,Peter Schirmacher, MD,## Michael Thomas, MD, PhD,† Rafael Rosell, MD, PhD,§ Federico Cappuzzo, MD,*** and Rolf Stahel, MD†††; on Behalf of the European EGFR Workshop Group. Consensus for EGFR Mutation Testing in Non-small Cell Lung Cancer. J Thorac Oncol. 2010;5: 1706–1713.
- Gray SW, Kim B, Sholl L, et al. Medical Oncologists’ Experiences in Using Genomic Testing for Lung and Colorectal Cancer Care. J Oncol Pract. 2017;13(3):e185-e196.
- Pujol P, Lyonnet DS, Frebourg T, et al. Lack of referral for genetic counseling and testing in BRCA1/2 and Lynch syndromes: A nationwide study based on 240,134 consultations and 134,652 genetic tests. Breast Cancer Res Treat. 2013;141:135–144.
- FDA Approved Drugs for Oncology, Drugs Approved in 2018. https://www.centerwatch.com/drug-information/fda-approved-drugs/therapeutic-area/12/oncology. Last retrieved December 2018.
- Vicki Leigh Keedy, Sarah Temin, Mark R. Somerfield, Mary Beth Beasley, David H. Johnson, Lisa M. McShane, Daniel T. Milton, John R. Strawn, Heather A. Wakelee, and Giuseppe Giaccone. American Society of Clinical Oncology Provisional Clinical Opinion: Epidermal Growth Factor Receptor (EGFR) Mutation Testing for Patients With Advanced Non–Small- Cell Lung Cancer Considering First-Line EGFR Tyrosine Kinase Inhibitor Therapy. Journal of Clinical Oncology: 2011 29:15, 2121-2127.
- Fouad Al Dayel. EGFR mutation testing in non-small cell lung cancer (NSCLC). Journal of Infection and Public Health (2012) 5, S31-S34.
- Do H, Dobrovic A. Limited copy number-high resolution melting (LCN-HRM) enables the detection and identification by sequencing of low level mutations in cancer biopsies. Mol Cancer 2009;8:82.
- Heideman DA, Thunnissen FB, Doeleman M, et al. A panel of high resolution melting (HRM) technology-based assays with direct sequenc- ing possibility for effective mutation screening of EGFR and K-ras genes. Cell Oncol 2009;31:329 –333.
- Do H, Krypuy M, Mitchell PL, et al. High resolution melting analysis for rapid and sensitive EGFR and KRAS mutation detection in formalin fixed paraffin embedded biopsies. BMC Cancer 2008;8:142.
- Yu J, Kane S, Wu J, et al. Mutation-specific antibodies for the detection of EGFR mutations in non-small-cell lung cancer. Clin Cancer Res 2009;15:3023–3028.
- Brevet M, Arcila M, Ladanyi M. Assessment of EGFR mutation status in lung adenocarcinoma by immunohistochemistry using antibodies specific to the two major forms of mutant EGFR. J Mol Diagn 2010; 12:169 –176.
- Ng J, Shuryak I. Minimizing second cancer risk following radiotherapy: current perspectives. Cancer Manag Res. 2014;7:1-11. Published 2014 Dec 17.
- Lopes GL, Vattimo EF, Castro Junior Gd. Identifying activating mutations in the EGFR gene: prognostic and therapeutic implications in non-small cell lung cancer. J Bras Pneumol. 2015;41(4):365-75.
- -C. Soria, Y. Ohe, J. Vansteenkiste, T. Reungwetwattana, B. Chewaskulyong, K.H. Lee, A. Dechaphunkul, F. Imamura, N. Nogami, T. Kurata, I. Okamoto, C. Zhou, B.C. Cho, Y. Cheng, E.K. Cho, P.J. Voon, D. Planchard, W.-C. Su, J.E. Gray, S.-M. Lee, R. Hodge, M. Marotti, Y. Rukazenkov, and S.S. Ramalingam, for the FLAURA Investigators. Osimertinib in EGFR Mutation-Positive Advanced Non-Small Cell Lung Cancer. NEJM. 18 Nov 2017.